Wednesday, August 31, 2005
Back Story-Thanks, 22q11 deletion, feeding tube
 There have been many things that have happened regarding Sophia's treatment since her heart surgery. And I would like to cover them all eventually but, the purpose of this blog was to allow people to keep up with Sophia's daily activities.
There have been many things that have happened regarding Sophia's treatment since her heart surgery. And I would like to cover them all eventually but, the purpose of this blog was to allow people to keep up with Sophia's daily activities.So I am going to comment on some of the challenges we have had, as well as, some of the joys and accomplishments in the future.
But first I would like to thank all the people that helped us during the time I have wrote about thus far. I am not going to put any names here, as I am sure some would not like to be named. But, there were several people who took care of our house and pets while we were in the hospital. There were many who brought us food at the hospital (as you can imagine hospital food gets old fast). There were many who provided emotional support and encouragement. And there were also many who helped with the financial concerns we had at the time. And there were also some who helped us care for Sophia while she was home.
I really want to thank all the family, friends, and coworkers that helped us through this incredibly difficult time. We could not have done it without all the help we received and we will forever be indebted to those who helped us.
I would also like to thank my spiritual teacher, Khachab Rinpoche, who came to the hospital and provided the blessings we all needed at the time. And also thanks to all the friends and strangers alike that provided prayers and wishes for Sophia's good health.
And of course, I have to thank Sophia's doctor's and nurses. Especially her cardiologist and Cardiac surgeon. They make it possible for our daughter to experience life.
Now for the catch up.
The first big thing I need to mention is Sophia's genetic diagnosis. Tests were done and it was determined that Sophia had what is called 22q11 deletion, often called DiGeorge Syndrome.
This was something we were not prepared for. We knew the heart condition was very serious, but, it could be repaired and Sophia would pretty much be normal. With this diagnosis, not only did we have to accept what would likely be a series of health problems to come, but also that it couldn't be repaired.
There is a long list of health problems associated with DiGeorge. But most kids do not have all of them. And so far Sophia has only shown evidence of a few. The heart condition is the big one. The feeding disorder I mentioned in the last post is another one. Sophia has had some developmental delay but at this point it is not clear how much of that is related to her heart condition and the development time she lost while in the hospital. For now, It seems her delays are within normal ranges. She was recently checked for a submucosal cleft palate and there is no evidence to indicate any type of cleft palate at this time. I will post much more regarding these issues in the future.
Since the time of discharge, we have had many doctors appointments, therapist visits, and even some surgery. I will mention the surgery first.
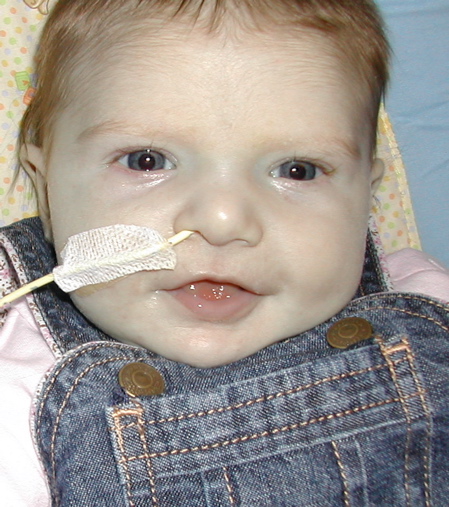
When Sophia was discharged she had an NG tube that was used for all of the nutrition she received. As she was not able to eat orally, she was given formula through this tube in her nose with an electric pump. When it became evident Sophia was going to eat in this way for some time, we decided this issue should be addressed.
The NG-tube was uncomfortable for Sophia and partially blocked Sophia's only good nasal airway (she has unilateral choanal atresia). So we decided Sophia would be better of with a G-tube. Here is a link dealing with tube feeding.
This surgery was much more routine than the heart surgery and Sophia is doing great with her g-tube. There was some adjustment time while everything healed. But now Sophia is gaining weight and is in the 50th percentile for height and weight. I will make future posts on feeding, Digeorge, and cardiology in the future as it becomes necessary.
I think I will try to give an overview of all the regular therapies Sophia receives in our home through a state agency called First Steps in my next post.
But for now I will say goodbye.
Thanks for reading. I look forward to your comments.
-Michael
Next Heart Surgery
I just wanted to make a quick note that Sophia will be having another major heart surgery on September 14th. I will give more details in a few days. But, this is a scheduled surgery and Sophia is not in any imminent danger.
-M
-M
Tuesday, August 30, 2005
Back Story- Surgery
Hi everyone. Sorry I missed posting for a couple of days. Thanks for the comments. It is really nice to hear from the people reading this.
So I left off with Sophia's welcome home party. It was really great, but Sophia seemed tired and slept through most of it. Looking at photos from that time now it is evident how blue she was. But at the time it was not.
The next morning we had a routine follow-up appointment with the cardiologist. He immediately said he thought she seemed bluer than she was at discharge from the hospital. He had some trouble getting an accurate reading of her O2 saturation (I explained O2 Sats in one of the children's hospital posts). I guess he didn't have the tiny probes they used in the hospital and he was having a hard time getting an accurate reading from Sophia's tiny fingers. He made a guess based on her color and suggested we go to the emergency room as a safeguard.
We went to the ER at the children's hospital and they hooked up the monitor and got a really low reading (50s). And decided that she should be admitted immediately. They established I.V. access and gave her oxygen and we were sent to the PICU (pediatric ICU), since Sophia's was no longer considered neonatal we did not go to the NICU this time. We had been out of the hospital just a couple of weeks at this point.
They determined that she would need surgery right away, but not immediately. They had decided they would do the Blalock Taussig shunt I mentioned before. They scheduled it for the next morning. All we could do was wait. Of course, if she got any worse they would operate immediately.
They explained the procedure to us and we signed all the authorizations. They explained she might need to be put on a heart/lung bypass machine that would function as these organs while they operated which would increase the possibility of complications.
The PICU was a slightly different environment than the NICU. She had a private room, but it was pretty open. The protocol to get in to the ward was similar to the NICU. The thing we noticed right away was that there seemed to be greater access to the doctors than in the NICU.
The next morning Sophia was prepared for surgery. She would have to be intubated and a ventilator would breath for her while she was under the anesthesia. The surgery was about three hours and everything went great. She did not require the heart/lung bypass machine. When we saw her, she was on the ventilator. She had a feeding tube down her throat. She was extremely swollen all over (from all the excess I.V. fluids she had received in the OR). She had about a three inch incision down the middle of her chest held together by staples. Just below the incision was an 1/8th inch diameter tube about 10-12" long with a bulb on the end that allowed fluid in her chest cavity to drain. She also had a catheter to collect her urine (she'd had a catheter in the NICU also).
Now we had to wait for her to wake up so the ventilator could be removed. Sophia had a real tough time with this. If I remember right, it was at least a couple of days before they even attempted to extubate her. The belief was that she was relying on the vent to breath for her. They called this "riding the vent." One of her doctors thought that she might breath on her own if it was removed . The analogy they used was "she would fly" without the vent. I think this was a comparison to a bird leaving the nest. This attempt failed miserably and she had to be reintubated the same day when it became evident she was not going to breath on her own.
She was given some respiratory treatments, medications and more time.
While she was on the vent, she had to be suctioned regularly to keep the airway clear and keep the vent working efficiently. This was a tricky thing and was quite scary to us. Sophia had what was explained to us as reactive vessels. I am not sure I remember the cause. But what this meant was that every time she was suctioned she would "clamp down" and her O2 sats would plummet. One time they dropped to about 35% which was terrifying to us and I think shook her nurse up quite a bit too. But, eventually she was able to be extubated and a new series of challenges presented themselves.
She was getting regular doses of narcotics to manage both her pain and to keep her sedated, which was especially necessary while she was on the vent. Mainly because of this reactivness I mentioned above. She received alternating doses of morphine and fentanyl. Once she was extubated these doses were tapered off in order to make her a little more alert. After these drugs were discontinued, it became apparent to us rather quickly that Sophia was not well. She couldn't sleep, she cried inconsolably and she was noticeably agitated. When we explained this to the nurse and suggested that we thought it was related to the narcotics, she said she seemed fine to her. The next day (this had continued through the night) a new nurse came in and noticed immediately that Sophia was exhibiting signs of narcotic withdrawal. The nurse the night before had been instructed to watch for this and report to the doctor any changes in her behavior. She had ignored our suggestions and not reported any of this to the doctor, who was not happy. In fact, he was noticeably angry. However, Sophia was started on a withdrawal treatment immediately that consisted of a methodone/ativan taper. It was a 15-day program. It was obviously not easy for us to accept that Sophia was a drug addict and not even 2mos old.
The next big obstacle was feeding and this has been a challenge to this day. Sophia went into surgery eating a normal volume of formula from a bottle like any other baby. After surgery she was not able to eat from a bottle and has not since. I can discuss this more in future posts. But the thing I will say here is, Sophia was discharged from the hospital with a feeding tube in her nose (NG tube) and a feeding pump. And after doing a swallow study it was determined that Sophia would receive nothing by mouth. Like I said, I will post more on this issue later.
Here is the summary. Sophia received a B-T Shunt. Her surgery was very successful and her recovery was quick.
She had many complications associated with narcotic withdrawal and a feeding disorder which did not exist prior to surgery.
After about a month of hospitalization, Sophia was finally released.
This is a very quick summary and I have left out much of the details. But, I will gladly answer any comments regarding parts of this I did not cover well. Just post them to the blog and I will respond.
More later-Michael
Saturday, August 27, 2005
Back Story-Welcome Home
 This will hopefully be a shorter post.
This will hopefully be a shorter post.So, we finally got to take Sophia home. It seemed like she was born months earlier, as so much had happened since then. But, now we had to do the newborn baby/first-time parents thing.
As this was not much different than bringing a healthy baby home, I won't spend a great deal of time on it.
Because of the schedule of the NICU and the constant noises and lighting, Sophia was quite confused as far as sleeping went. Now I know that many babies sleep at weird times and it rarely is in congress with the parents schedule. But what I think was unique about Sophia was that she was very upset by silence. She had become so accustomed to light and noise that when it was gone she got scared and cried. So we had to sleep with a lamp on. And we had a small humidifier in our room that emitted enough white noise to keep Sophia pacified.
The sleeping arrangement we decided on was a bedside bassinet. This bassinet attached to the side of our bed, which made it almost like a small extension on the side of our bed.
She was fed every three hours around the clock. Which was a little adjustment. In the NICU, if we were especially tired or preoccupied with other concerns a nurse could feed or change Sophia. We however rarely took advantage of this because it was very fulfilling to feed Sophia and we did it at almost every opportunity.
My wife continued to pump her breasts with the hope her milk might come in without all the stress of the hospital. This unfortunately never really happened and her production was very little. And after a week or so, it became evident that Sophia was going to be formula fed.
We didn't sleep for what seemed like forever. I am sure this is not uncommon with babies in general. But we of course had no idea it would be that bad. Patty's best friend was here from Florida to help out and I am not sure we would have kept our sanity without her assistance. She has two children of her own and her experience was invaluable.
The only other thing that was a challenge for us was Sophia's medications. There were of course many and scheduling and preparing them while trying to manage her sleeping, eating, peeing, and pooping was incredibly challenging.
But soon we got pretty good at all this and a routine was emerging.
We decided it would be a good time to have all our friends and family over to meet Sophia. Throwing a party while also trying to master all this mom and dad stuff shows the degree to which our sleep deprivation had effected our judgment. But, because of the nature of the NICU only a few of our friends and family had even met Sophia, who was now almost 6 weeks old. So we had the party and it was really great. I think we all really needed it and so many of our friends helped with everything that we managed to not go totally mad from its planning and execution.
Thanks for reading Sophia's story. I will write more tomorrow. And like I said in the last post, comments are appreciated.
-Michael
Friday, August 26, 2005
Back Story-Children's Hospital (cont'd.)
 Thanks to anyone checking in. Please feel free to leave comments. It is nice to know if anyone is reading these posts.
Thanks to anyone checking in. Please feel free to leave comments. It is nice to know if anyone is reading these posts.So when I left off last time, the side effects of Sophia's treatment with prostaglandin was causing us a great deal of anxiety. But of course we believed this was all that was keeping her alive.
The next major step in her treatment was to get a more accurate diagnosis. This required a heart catheterization. This was done by inserting a small catheter in the top of Sophia's thigh near her groin. It would be carefully guided into her heart and a contrast dye would be injected. After this video pictures were taken that would show the way the heart and its major vessels moved the dye in and around her heart. This would give surgery and cardiology a clearer picture of her heart's anatomy. This was scheduled and in the meantime we focused on feeding Sophia.
As I had mentioned in an earlier post, Sophia latched on and breastfed immediately after her birth. And Patty and I had no intention of feeding her anything other than breast milk.
The problem was that Sophia's heart prevented her from having the energy necessary to breast feed. So we went for the next best thing and Patty started pumping her breasts. She met with a lactation specialist who helped her in every way possible but her milk never came in the way it should. Even though she religiously pumped every three hours around the clock, she was not able to produce the volume necessary to provide all of Sophia's nutrition. In the beginning, there was enough, but soon it became necessary to supplement with formula. This was the first of many blows to our first-time parent idealism.
The experience of feeding Sophia, even though it was with a bottle, was the greatest feeling ever. Like I mentioned above, there was not enough breast milk to feed her that exclusively. But every drop my wife was able to pump was given to her. And no matter how little that was, Patty never gave up and continued to pump the entire time we were there.
It was such a helpless feeling to be going through this and I think providing even the tiniest amount of breast milk made her feel like she was contributing to Sophia's health.
The catheterization was our first experience with a surgical procedure for Sophia. The risks were pretty small but it was still difficult. And of course we had just a vague idea of what they might find. When we received the results they were received in a variety of ways. For Patty and myself it confirmed that her heart had some serious defects and revealed some that had not been mentioned before. We were informed that there was a good possibility that the defects could be repaired but would require a series of open chest and open heart surgeries.
Cardiac surgery would be consulted and the next course of action would be determined. They explained that there was no evidence of the "patent ductus" I mentioned in an earlier post. It was determined instead that a series of small collateral vessels were carrying blood to the lungs instead. Therefore, the treatment with the prostaglandin seemed unnecessary and was discontinued. The specific diagnosis she was given was Tetralogy of Fallot with Pulmonary Trunk Atresia and the small collateral vessels I mentioned above.
After cardiac surgery reviewed the film, they decided that Sophia would need a surgery to either gather these collaterals into a more substantial vessel and connect them to the heart or to do a surgery called a Blalock-Taussig Shunt.
But both would require the vessels to grow to a workable size for the surgeons.
Back in the NICU, we were still dealing with feeding issues. Sophia was doing pretty well with the bottle but was not taking the volume she should. It would be necessary for us to get to a target volume in order to be released. With the prostaglandin gone, the apnea was much better and Sophia seemed to be a little more awake. Soon she was taking the necessary volume of formula. My wife continued to pump.
The plan was that Sophia would go home and regularly visit Dr. O'Laughlin her cardiologist. Once the vessels were large enough or something else made surgery necessary, she would return for surgery.
But, before we could go home we had to do a PC(Parent Care) status night. This meant that we would have a room in which we could stay overnight with Sophia and all of her care would be our responsibility. This was daunting with all that had happened up to this point. But we were ready to take our daughter home. There were two things that were really good about this night. First, we could stay in the room and even sleep. The NICU policies prevented parents from sleeping in the pods. You could stay all night but if you fell asleep they would kick you out.
Second, and this is huge, NO MONITORS. The funny thing is that everybody reassured us that she would be OK without them and that if we had to put her back on them she couldn't go home. But, we were thrilled to be rid of the thing that had driven us mad for weeks now.
There were no alarms and no slowly ascending and descending numbers. I suppose we could have stopped paying attention to them a long time ago. But I think we had become seriously dependent on those little numbers to tell us how things were going. But now we were free.
The night went fine and we were released the next day. We were there for three weeks and were so glad to go home.
More tomorrow-Michael
Thursday, August 25, 2005
More Back Story-Children's Hospital

I thought I should mention that Sophia is presently doing very well. But, she is scheduled to have a major surgery in mid-September. As that date approachs, I will post more on current events. But, I really want to continue with the back story because it is helpful for me to write about it and also it creates a context for future posts.
Again, I am sorry for the long posts but I really want to get this story in. I appreciate anyone who is interested enough to read about this, and I hope it benefits others in some way.
So early in the morning after what seemed like the longest night of our lives. An elabortate transport was underway. A team of paramedics and an abulance moved my daughter to the NICU (Neonatal ICU) at the children's hospital. My wife, Patty, had to stay at the hospital where Sophia was born. She had to heal from the substantial tear she got during delivery. I am sure this was an incredibly difficult time for her. I followed the ambulance to the hospital with my mother.
Soon we arrived at the hospital where they were well prepared to recieve Sophia. The NICU was like no place I had been to before. For that matter, this hospital was very different than what I had experienced before. I had never been to a children's hospital and had no idea what to expect. I think I thought it would be a depressing experience because there isn't much that is sadder than sick children and this was like a mini-city of sick children. But instead I found it kind of inspiring. I will try to elaborate on this more later.
The NICU was divided into five or six "pods" each with about a half-dozen babies. Most were premature, but there were a few other "heart babies". The assigned spaces in the pods were probably about the size of a parking space, open on three sides with a warmer for the baby and a couple of chairs.
There were a ton of rules. It was a major scenario to get in the place. From the outer lobby, you had to press a buzzer. An attendant inside who could see you on a monitor would buzz the door open and let you in. Once inside, there was desk where you would have to sign in. After you signed in you were given a badge that showed your relationship to the patient and the pod to which they were assigned. There were only two badges per patient, because only two people were allowed back at bedside at a time. One of the two had to be a parent. Though they did allow us to designate others who could go back without us (grandparents).
Once you were signed in, there was an elaborate hand-washing ritual. You were buzzed through another set of doors. Inside was a small room with a trough sink. Above the sink were individually packaged brushes with medicated soap in them. You were to scrub your hands with the little brush for two minutes and dry your hands with paper towels. This had to be done everytime you entered the NICU.
After you were in you could go to see your baby, but you were not allowed to stray at all from that course. Privacy was a very big concern but the pods were open environments, which made this difficult to enforce.
When I first got there Sophia was assigned two RNs. Most of her care was handled by a pediatric resident, who answered to an attending physician. They rounded twice a day around shift changes.
Another rule was that no visitors were allowed including parents at shift change. I think this was another privacy policy, since the nurses had to pass on all pertinent info about every patient to the nurses coming on for the next shift. These later proved a good time to get something to eat. Parents were encouraged to be there when the doctors would round. This was something I always made an effort to attend. It was a good time to find out the details of Sophia's treatment as well as voice our concerns and wishes regarding her care.
Patty arrived two days after Sophia was transported to the children's hospital. By this time I was pretty well aclimated to the environment, but she was of course very disoriented by the experience. I am sure her main concern was to hold Sophia as they had been seperated from shortly after her birth. In the time she was seperated, they had placed several I.V. lines and monitors for showing her heart rate, respiration, and oxygen saturation. She had been on oxygen for much of the time they were apart but I think she was on room air or just what they call blow-by oxygen at this point. She had a large I.V. in her head that allowed them to give her nutrition interveinously. I am sure it was a pretty dramatic scene but she was doing much better than the last time Patty had seen her.
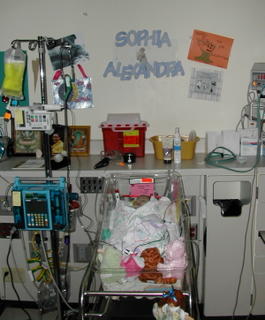
During her time in the NICU, she was still being treated with the prostaglandin I mentioned in the last post. In fact it was the doctor's assumption that it was the only thing keeping her stable. Unfortunately, there were some pretty substantial side effects associated with this treatment. The worst of which was apnea. Apnea is when the respiration becomes so depressed breathing just stops. This made it impossible for us to relax. The monitors I mentioned earlier became an obsession for us.
The most important of the measurements on the monitor was the one called O2 Saturation, or Sats for short. Because of Sophia's heart condition, her sats would range from 65-75%. Normal is around 99-100%. This was an indication of the oxygen in her blood. Now, the nurses would set a range on the monitirs and if she went above or below certain numbers an alarm would sound. Everytime an alarm would sound, she would have to be stimulated to get her to breathe or given oxygen or have her airway cleared of mucus/secretions. There were times the sats dropped below 45%. Like I say this number became our obsession. It was our indication of whether Sophia was doing good or not. We started calling it "Sat TV", but it was truly terrifying.
I will continue this tomorrow.
Thanks for checking in-Michael
Wednesday, August 24, 2005
Back Story-Hospital
In this post, I am going to continue the story where I left off yesterday.
I apologize for the long posts but I want to get all this history down so people will be able to understand the context of this weblog.
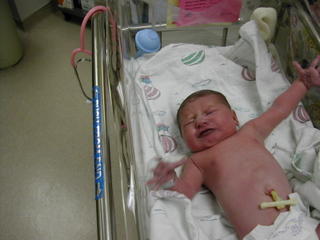
So as I had explained in the last post, Sophia was born at 4:32pm on October 27th, 2004.
And all seemed to be fine, other than the anxiety I had about caring for and nurturing this small person we had just ushered into the world. And my wife's total exhaustion from pushing. As soon as Sophia was all done being evaluated she was given to my wife and she immediately latched on and began to breastfeed. Awesome.
Once we were moved to our room, we got settled in and were informed that Sophia would pretty much be our responsibility to care for, but we would get some assistance and instruction from the nursing staff. And, we could utilize the nursery in the wing if we had too. Soon I got to assist in giving Sophia her first bath while my wife rested. Shortly after this we noticed Sophia was having some issues breathing. Mostly just a stuffy nose as far as we could tell. So I called the nurse and she thought maybe she seemed "a little dusky" but also thought it was something in her nose. She suggested we take her to the nursery to have her nose suctioned and let them keep an eye on her. Not long had passed and the nurse came back and informed us that they were not having much success clearing her nose and said they were going to send her down the hall where they had a better suction.
Now, this term "a little dusky", which in this context means a little blueish, was the one that would change things for all of us. Apparently the place with the better suction was the Neonatal ICU. It was getting pretty late in the evening by this time and all of the visitors we had had were gone and we were pretty anxious about what was happening but assumed it was no big deal. After all, this was all new to us.
Fortunately, there was a great neonatalogist on call that night. He thought that there may be something more to this than just some junk in her airway. So he ordered a chest x-ray and he wasn't sure but suspected a possible problem with her heart anatomy. He came down to our room and explained this situation to us and of course we were incredibly distressed by the news. All you want to hear after a very long time of contemplating having children and nine months of pregnancy is the baby is healthy. I think we would have been freaked out by some minor problem. To hear that her heart may not work right and may not even be anatomically correct was devastating. He informed us that he had called in a consult from a pediatric cardiologist and that he would be there anytime.
It was really late by now. I think it was 2-2:30am. Around 3am, we met Dr. O'Laughlin, Sophia's cardiologist. He explained everything to us in great detail and even drew us diagrams.
But most importantly, he had this really great way of talking to us that somehow made it seem like a workable situation.
He explained to us, that he had done an echocardiogram on Sophia. Which shows not only the anatomy of the heart but also the direction of the blood flow. He told us that the what the neonatalogist, who had suspected the major vessels to the heart were reversed, was incorrect. And that he instead suspected that her pulmonary arteries were not properly moving blood to her lungs to get oxygen. He also explained to us that when babies are still in the womb, they have a small "duct" that allows the blood in the heart to mix. I think this is because the lungs are not necessary in utero because the mother supplies the oxygen to the baby. This patent ductus is usually between the aorta and the pulmonary arteries. Shortly after birth, this ductus closes and the heart functions as it should with no mixing of oxygen rich and oxygen spent blood. He explained to us that because there was no proper connection from the heart to the lungs as this ductus began to close Sophia became "cyanotic" or blue. So, the plan was to give Sophia a medication called prostaglandin that would keep the ductus "patent" or open. And then transfer her to the local children's hospital when possible the next day.
At this point, we called our parents and woke them to explain the situation. We were then allowed to go see Sophia who had been away from us for several hours. I wheeled my wife down the hall in a wheelchair and we had no idea what to expect. And I don't think we could have prepared for what we saw anyway.
Sophia looked completely different than earlier that evening. She was pale and in an oxygen tent. She was breathing very short labored breaths and was on all kinds of flashing and beeping monitors (which we would later become very familiar with). At that point, I think my wife and I both were not sure she would make it through the night. They asked if we would like to hold her and my wife really did. So they affixed an oxygen mask to her and my wife held her and sang to her.
More tomorrow.
-Michael
Tuesday, August 23, 2005
Back Story-Pregnancy and Delivery
Before I get to more recent events in Sophia's story, I thought I would spend the next few posts giving an abridged history starting about a year ago.
My wife Patty and I have been married for 10 years and had waited until the last few years to try to have a child. Once we made that decision, it was 18-24 months before Sophia was conceived.
Patty had a pretty rough pregnancy. She had severe morning sickness early in the pregnancy which caused her to lose a great deal of weight. She was later diagnosed with borderline gestational diabetes, preeclampsia, and a condition called polyhydramnios (which is an excess of fluid in the womb). Because of this she spent the last three months of her pregnancy at home on bed rest. And also because of this she had several extensive tests including four level 2 sonograms and biweekly stress tests. In all of these tests there was no indication of any problems with the baby. Even the sonograms which included an echocardiogram of the baby's heart showed no structural heart defects.
All this aside, as you might imagine we were filled with anticipation of the possibilities this new life would bring. We did loads of research and read many books about development, feeding, diapers, etc. All with the expectation that we would have a healthy baby. We had all kinds of aspirations of how everything would be once she got here. And put everything in place to make everything perfect.
We chose a room to be the baby's nursery, and I spent several months painting murals on the walls and ceilings. I painted blue sky with fluffy clouds on the walls and night sky complete with glow-in-the-dark stars on the ceiling. We bought furniture and books and prepared to meet her every wish and do our best to fulfill her dreams.
We researched breastfeeding and cloth diapering, and we purchased cloth diapers and a breast pump for when my wife would return to work. We took some classes the hospital provided and knew we had prepared for everything as well as we possibly could.
When Patty's pregnancy had reached term and Sophia was still not here. We decided because of the complications to the pregnancy to schedule labor inducement one week after the due date. We had discussed it and my wife intended to have a completely natural delivery. We checked in the hospital on 10/26 at around 9pm and the process of inducement was begun.
After a night of what we now know were mild contractions, my wife's doctor manually broke her water at 7am. It wasn't much after that active labor started and with it came the real contractions. At this point, all bets were off and my wife immediately decided to have an epidural block. Thanks to an experienced labor/delivery nurse, who new that three emergency cesarean sections had just been decided, anesthesia was rounded up immediately and the incredibly tense administration of the epidural began. If the nurse had not been so on top of things it would likely have been over an hour before anesthesia would have been available. After anesthesia did its thing and I recovered from nearly passing out from the tension, Patty got some much needed rest. I don't think I slept much at all the whole time we were at the hospital.
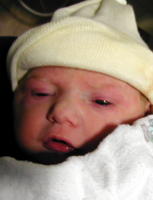
At around 3pm my wife was fully dilated and the delivery was getting started. My wife and I kept asking about the doctor and the nurse explained that they don't get there until the baby is ready to deliver (last few minutes). I think it was about 4pm when my wife started pushing. It was the most amazing display of will and strength I had ever seen. When the doctor came in she began suiting up with layer upon layer of protective garments, masks and shields. She had remembered the incredible amount of fluid my wife was carrying. And once Sophia's head was born the delivery room was flooded beyond anything I think anyone expected. Shortly after that her shoulders were slightly rotated and out she came. Apparently there was some concern that the fluid had some stool in it, and because of this Sophia was whisked away to have her airway cleared in order to make sure none was aspirated (which would cause a respiratory infection). But soon Sophia was crying and was evaluated as perfectly healthy. The doctor stitched up my wife and within a couple of hours we were moved from the delivery ward into our room.
To be continued...
-Michael


