Friday, September 30, 2005
Day 5-PICU-chest closed
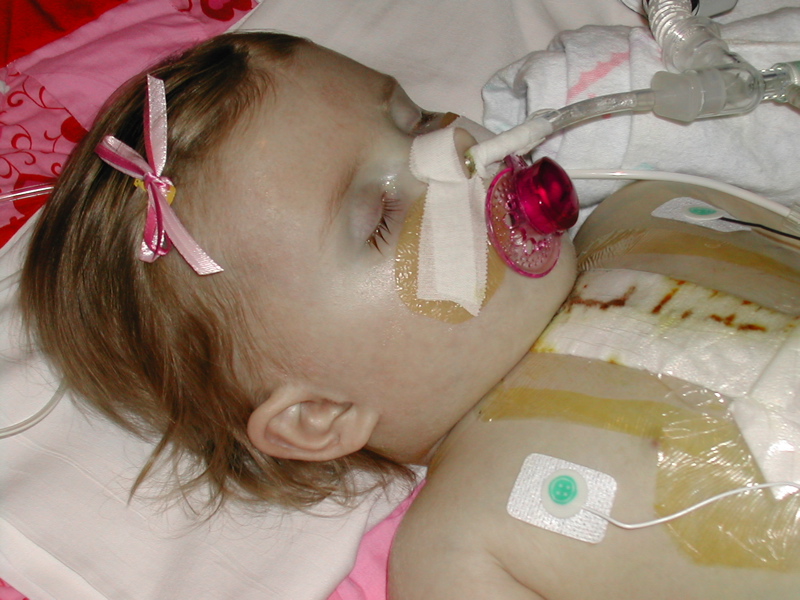
We have had lots of progress since yesterdays post.
Last night, around 1am, the nitric oxide was shut off.
And this morning, the surgeon came in and closed Sophia's chest.
They have reduced her Fentanyl and Versed, which were at very high doses to keep her sedated. And they shut off her Vecuronium (a paralytic). This should allow her to wake some and begin to move.
She is still on the ventilator. But we are progressing toward getting rid of it as well.
She is also on a small dose of a vaso-dilator called Milrinone that keeps the pulmonary vessels opened up. And a small dose of Epinephrine, which I think is somewhat like adrenaline.
Sophia has tolerated all of this quite well.
I will post as there are changes thanks for the comments. It means a lot to us to hear from you.
-Michael
Thursday, September 29, 2005
Day 4-PICU
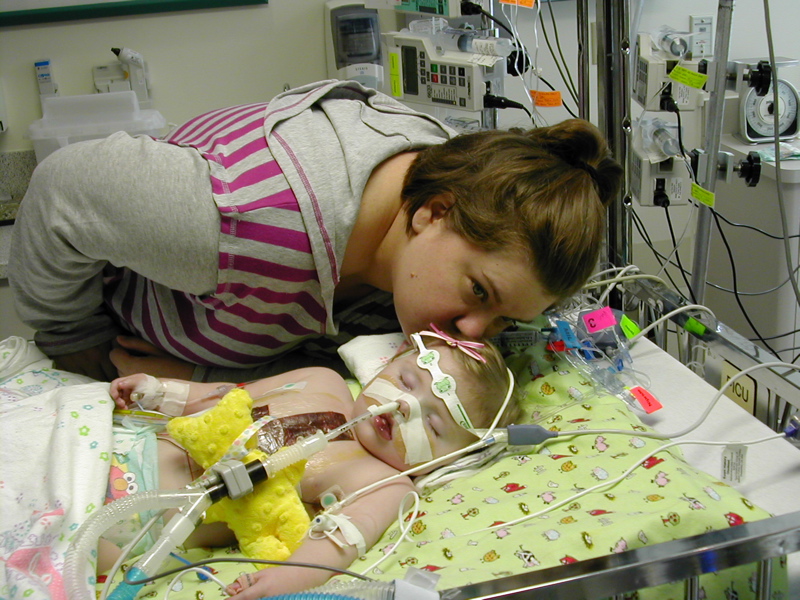
Sophia had a good night.
Her swelling and fluid retention is much reduced.
They have weaned her oxygen to 50% and are weaning her Nitric Oxide (a respitory support).
They are not going to close her chest today. But, they will likely close it tomorrow.
She has had a low grade fever. They drew some cultures and one came back positive for a slight bacterial infection. They are adjusting her antibiotics to deal with it. But her fever is down.
Over all she seems much better today. We hope she continues to progress the way she has so far. I will post again sometime tomorrow or if anything changes.
Hopefully, they will close her chest tomorrow so we can start to progress toward waking her and getting her off the ventilator.
Thanks for the comments on the last post. Please keep them coming. I am sorry I am not able to respond to them at this point. But if you have a specific question regarding her treatment and I am able to answer it I will try. You can post comments directly to the blog entry by clicking the comment link directly below it or use the email link below my profile to send email directly.
Thanks-Michael
Wednesday, September 28, 2005
Update-Day 3 PICU
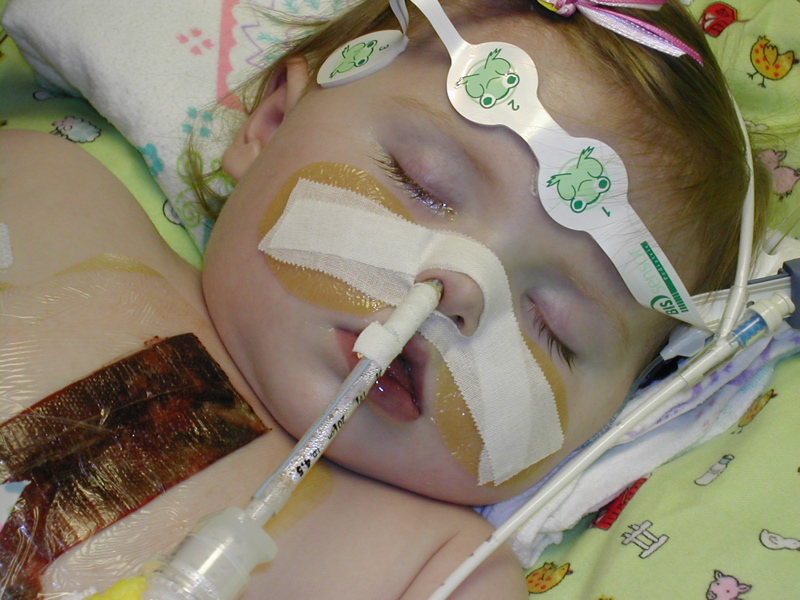
Sophia is still pretty unstable but doing better. Her main issue since surgery has been related to pulmonary hypertension. I think this is caused by a combination of the cardiac repair and the stress of being on the heart/lung bypass machine during surgery(I think I neglected to mention bypass in the last post about the surgery, sorry).
She is still completely sedated and on the ventilator. They probably will leave Sophia's chest open another day at least. There are no big changes planned for today. But, I will post if anything comes up.
As the details change quite frequently, it is impossible for me to post every change but I will try to give everyone a general idea of her condition at least once daily.
Thanks-Michael
Tuesday, September 27, 2005
Surgery Details
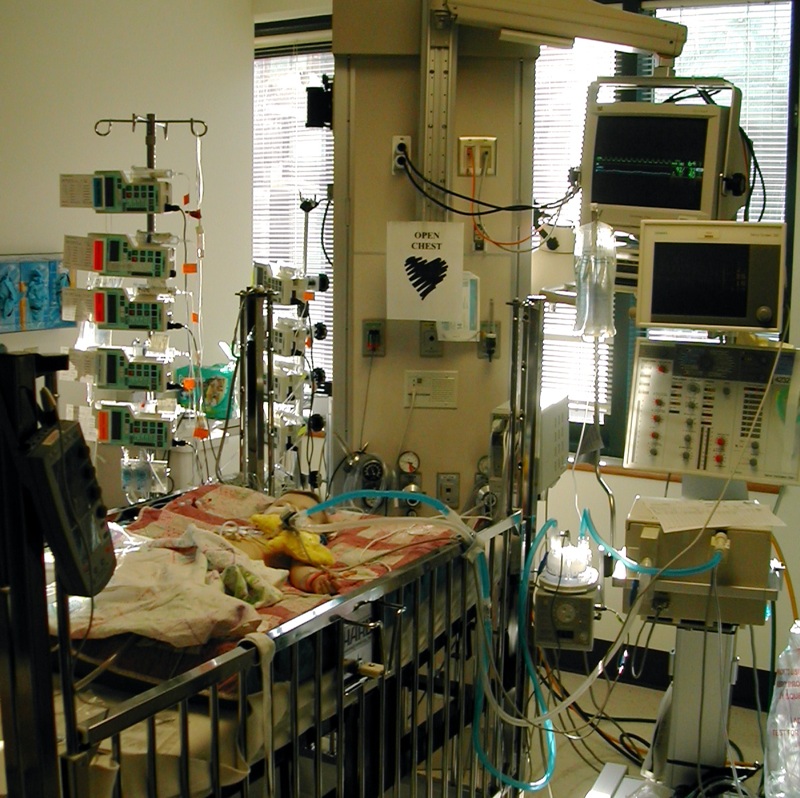
Hi everyone.
I have posted some pictures on the last two posts.
Here are the details I know so far regarding Sophia.
As I stated in previous posts, the goal of the surgery yesterday was to take down the B-T Shunt, unifocalize the multiple aorto-pulmonary collateral arteries (MAPCAs), place a right ventricle to pulmonary artery conduit, and close or reduce the VSD.
The shunt was removed no problem. There was a little scarring they had to deal with to get to it but it was successful. Of the MAPCAs there were a few that had grown quite substantially. They were successfully brought together and joined to the pulmonary artery. I think the surgeon said he even managed to successfully join one that was only 1mm diameter.
The RV to PA conduit was also done successfully.
The VSD was neither reduced or closed. Here is why.
The last cardiac catheterization revealed substantial growth in the PAs. What it did not reveal, was the vessels entering the lungs were still very small. This creates a sort of bottleneck which does not allow the amount of blood the heart pumps to easily enter the lungs. As a result, the VSD had to be left open to relieve stress the right ventricle would experience which could cause it to fail. By not closing the VSD, not only will it be necessary to have a future surgery to do so, but Sophia will still have less than optimum blood oxygen saturation.
At this point, we do not know what will happen regarding this situation and are focused on her recovery. But basically the pulmonary vessels will need to grow or be opened via cardiac cath at a later time.
Lastly, Sophia's chest was not closed after surgery. This is because there is a possibility of swelling that could impair the function of the heart and lungs. It should be closed in the next day or so in her PICU room.
This is what I know so far. I will continue to post short updates as I am able. I will post photos to the Flickr! page, when I am able to get home. There are a few there now.
Thanks to all who have supported us through this. Please send us emails and comments.
Thanks-Michael
Day Two-still critical
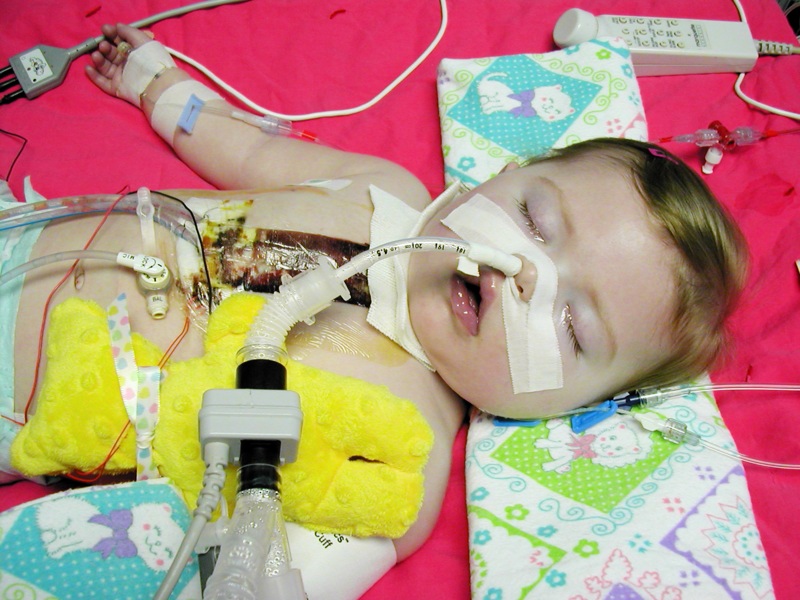
Sophia is doing better today, but is still critical. Her oxygen levels are key to her success at this point. She is of course intubated and a ventilator is doing her breathing for her. She is receiving many medications I will not list here. But I will say she has close to a dozen medication pumps. She is receiving clear fluids intravenously. She is getting versad as a sedative and fentanyl for pain management. She is also getting a drug that paralyzes her and allows her to relax while things adjust. I know that is very vague, but it is the best I can explain it right now. She is getting a respitory treatment called nitric oxide that helps to dilate her pulmonary vessels. This will allow her to more efficiently oxygenate her blood. She is also getting oxygen through her ventilator. They have begun to wean both of these, oxygen and nitric oxide. They have left her chest open to allow for swelling and will close it when she needs less respitory support. The cardiac surgeons and her cardiologist are encouraged by her progress since yesterday, but she still has a long way to go. Her care is being managed by an Intensive Care doctor.
I will try to post some pictures and an explanation of what the surgeon found during surgery either later this afternoon or tomorrow.
Please keep checking in. And please send your thoughts, feelings and comments. Hearing encouragement really helps in a situation like this.
Thanks-Michael
Monday, September 26, 2005
Sophia is Out of Operating Room
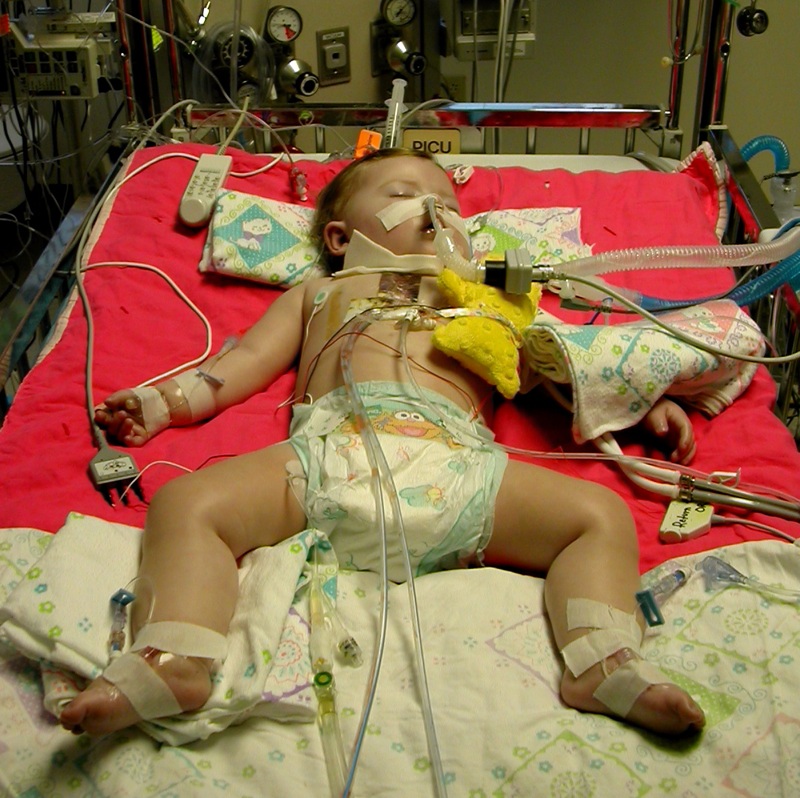
Sophia is out of surgery and the repair was successful.
Unfortunately the vessels in her lungs are a little reactive and her oxygen saturation level is still quite low (currently 60%s).
The next 24 hours will be critical. All we can do now is wait and hope for the best.
I will try to post more tomorrow.
-Michael
Sunday, September 25, 2005
Surgery in the Morning
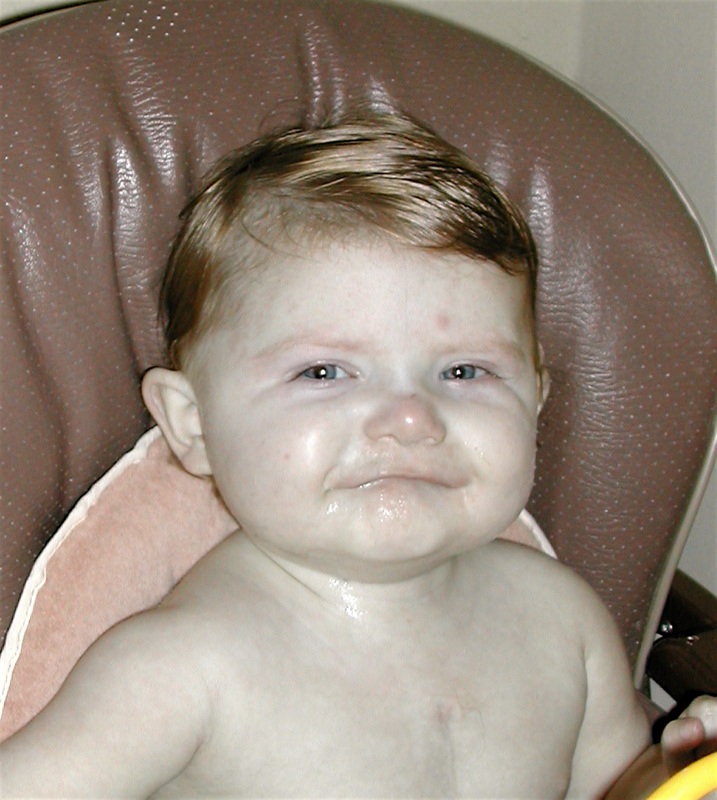 Surgery is at 7:30am tomorrow.
Surgery is at 7:30am tomorrow.I just gave Sophia a bath with some antiseptic soap provided by the hospital. She cannot eat past midnight so we are going to feed her at 11:30pm. She can have clear fluids until 3am. So she will have some pedialite at 2:30am. We are packed for the hospital and have made arrangements for the house and pets. We have to be there at 6am, so we will probably leave the house at 5:30. The surgery will likely last several hours.
Please keep Sophia in your thoughts and prayers.
I will post a short note once Sophia is out of surgery.
-Michael
Friday, September 23, 2005
Surgery Details
 We had our pre-op appointment today at the Children's Hospital. It went pretty well. We went over medical history and met with the surgeon. They got weight, height, and vitals. They also did chest x-rays, they took blood and urine, and did an EKG.
We had our pre-op appointment today at the Children's Hospital. It went pretty well. We went over medical history and met with the surgeon. They got weight, height, and vitals. They also did chest x-rays, they took blood and urine, and did an EKG.Sophia was pretty fussy and tired by the end. We were there 4.5-5 hours.
Like I said, we met with the surgeon and some of his staff. I thought I would post some diagrams of Sophia's heart and try to relay the details of the surgery. Here is a link regarding normal heart anatomy to use as a reference.
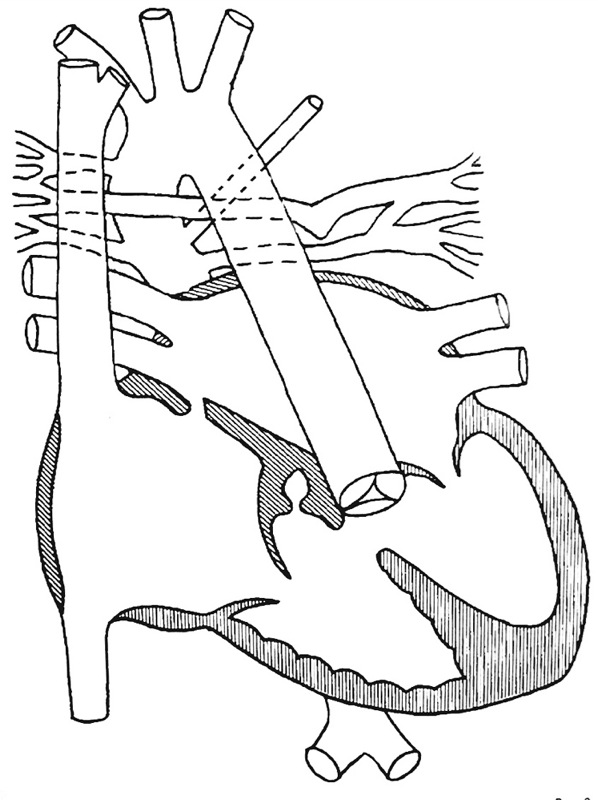
The line diagram to the left is what Sophia's heart was like at her first catheterization. In other words, there is no repair in this image.
Things to note:
If you look at the lower left chamber of the heart (the right ventricle or RV), the pulmonary valve is incomplete and does not connect to the pulmonary arteries (PA). This is called pulmonary trunk atresia. Also there is a substantial hole just below and to the right of the missing valve. This is called a VSD or ventricular septal defect. You might also notice tangled amongst the aorta and existing PAs, there are several small vessels that are connected in various places between the aorta and the lungs. These are called MAPCAs or multiple aorto-pulmonary collateral arteries. And if you are really perceptive you will notice the aortic arch is reversed from its normal direction.
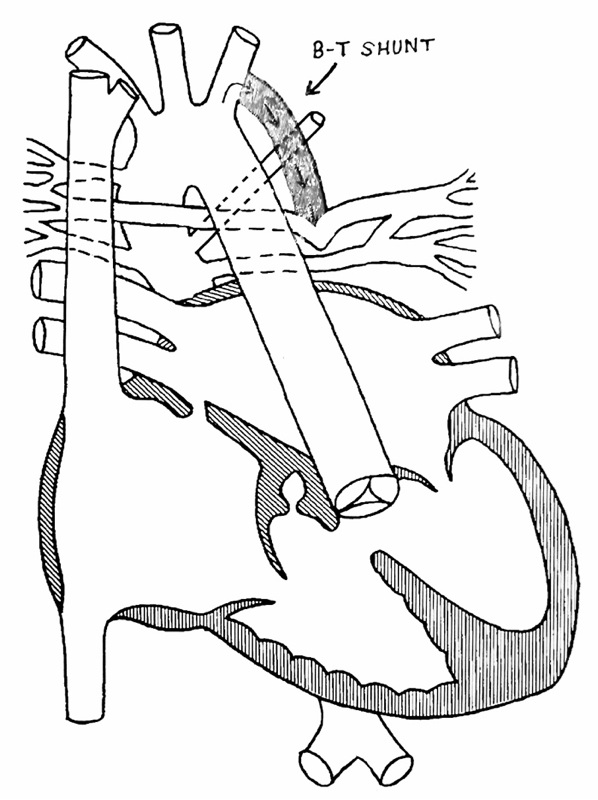
The next image shows the first repair called a Blalock-Taussig Shunt. This was done in November 2004, and I have written about it in a previous post. The repair is shown in gray. The purpose of this repair was to redirect the blood, returning to the body through the aorta, back to the lungs through the PAs (shaped like a seagull).

With the repair on Monday, the shunt will be removed and a conduit will be placed from the right ventricle to the pulmonary arteries.
This is called a RV to PA conduit. It is sourced from a cadaver donor. It will have a valve that allows the blood to flow in only one direction. This is not a permanent repair in the same way the shunt was not. Though it approximates the natural anatomy of the heart, Sophia will eventually outgrow it. There is also the possibility the valve will wear out. It should, however, last until age 7-10 given the valve lasts.
Also during the surgery, the MAPCAs will be unifocalized. This means they will be gathered together and connected to the PAs to allow them to bring blood to the lungs. In Sophia's situation these vessels are not servicing any part of the lungs that the PAs do not reach. This makes it less crucial they all be used. But, the surgeon is going to try to use them all.
Finally, the surgeon is going to either reduce or close the VSD. This will depend on the size and condition of the PAs and MAPCAs. Let me try to explain.
Because of the existing defects, the right ventricle has to pump pretty aggressively to move blood where it needs to go. With the repair, all that pressure will be directed to the PAs. If they are too small, the pressure could cause problems for the repair. In this case, the VSD offers a sort of relief valve. If it is necessary to have this relief the VSD will be reduced, if not the VSD will be closed. If the VSD were not closed, I am not sure if they would close it until they needed to repair the conduit later.
Below is an estimation of Sophia's heart after the repair.
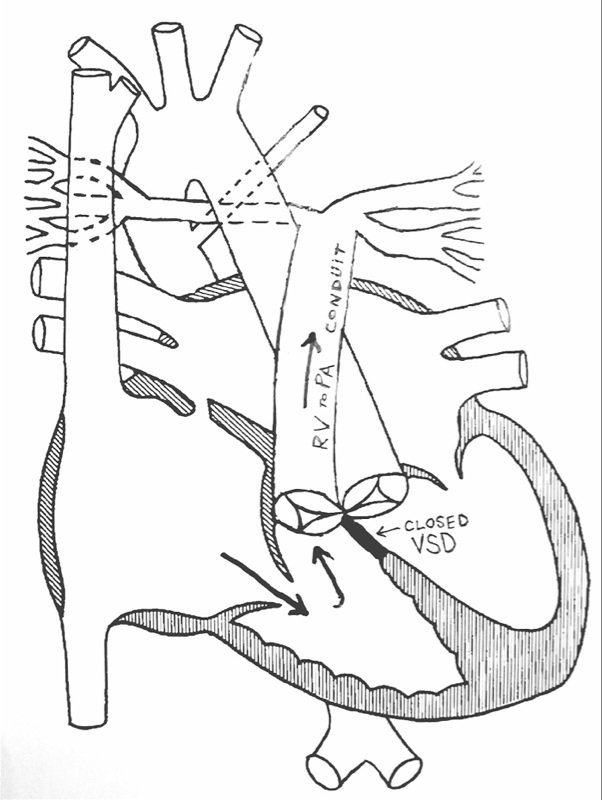 We are to arrive at the hospital at 6am on Monday. Surgery will be at 7:30. Anesthesia will put Sophia under using gas. She will then get 2 I.V. lines and an arterial line. They will put a breathing tube through her nose and into her windpipe. Then she will be hooked to a ventilator and the rest of the anesthesia will be administered. After this, the surgery will begin. It should last 4-6 hours.
We are to arrive at the hospital at 6am on Monday. Surgery will be at 7:30. Anesthesia will put Sophia under using gas. She will then get 2 I.V. lines and an arterial line. They will put a breathing tube through her nose and into her windpipe. Then she will be hooked to a ventilator and the rest of the anesthesia will be administered. After this, the surgery will begin. It should last 4-6 hours.Some of the concerns related to the surgery are outlined below. First, there is likely lots of scar tissue from her first surgery. This will have to be removed in order to give the surgeon access to the heart. This is of course a bleeding risk.
Another major risk is the heart/lung bypass. This is a machine that does the work of the heart and lungs while the heart is stopped for the surgery. This machine creates a sort of shock to these systems. And as a result there is much swelling and spilling of fluids into the tissues of the body.
Beyond that there are many other risk associated with the mechanics of the surgery and other general O.R. risks. We were told the risk of death is about 10%. This is obviously not as low as we would like. But the benefits far out weigh the risks.
This is a very general sketch of the procedure. And of course, not being a doctor myself, I am doing my best to be accurate. I will however make some errors in communicating this stuff. I will post more details as they are available. But, I wanted to give everyone an idea of what was going to happen. Check back after surgery, Monday night, I will try to post regarding the outcome.
-Michael
Thursday, September 22, 2005
Partners of the Heart
Hi.
I wanted to post a quick update.
Sophia has a pre-op appointment tomorrow. I will post the details of her surgery in the afternoon.
 I wanted to also recommend a documentary about Vivien Thomas and Alfred Blalock. These two men invented the surgery that Sophia has already had. Not only was it the very first heart surgery ever. Vivien Thomas(pictured above) was a black man in the segregated south and had only a high school education.
I wanted to also recommend a documentary about Vivien Thomas and Alfred Blalock. These two men invented the surgery that Sophia has already had. Not only was it the very first heart surgery ever. Vivien Thomas(pictured above) was a black man in the segregated south and had only a high school education.
The documentary called "Partners of the Heart" is a PBS American Experience project. We got it through netflix.
There is a website here.
Check out the operation link. It illustrates very clearly the Blalock-Taussig Shunt procedure.
-Michael
I wanted to post a quick update.
Sophia has a pre-op appointment tomorrow. I will post the details of her surgery in the afternoon.
 I wanted to also recommend a documentary about Vivien Thomas and Alfred Blalock. These two men invented the surgery that Sophia has already had. Not only was it the very first heart surgery ever. Vivien Thomas(pictured above) was a black man in the segregated south and had only a high school education.
I wanted to also recommend a documentary about Vivien Thomas and Alfred Blalock. These two men invented the surgery that Sophia has already had. Not only was it the very first heart surgery ever. Vivien Thomas(pictured above) was a black man in the segregated south and had only a high school education.The documentary called "Partners of the Heart" is a PBS American Experience project. We got it through netflix.
There is a website here.
Check out the operation link. It illustrates very clearly the Blalock-Taussig Shunt procedure.
-Michael
Wednesday, September 14, 2005
Now We Wait.
Hi all.
I went back to work today. And though I was not thrilled, it was better than agonizing in the surgery waiting room while they cut on Sophia. Sophia's surgery being postponed has me thinking about how mentally prepared I am for it. I think yesterday was a good exercise/dry run for what is inevitable. And though I cannot think of any preparation that I haven't already done. This has left me a little better prepared than I would have been if we were having surgery today.
The hardest part of it, is that Sophia is doing better right now than she ever has. This is great in almost every way that I can think of. But, it prevents me from dealing with the surgery in a way that would be easier. It isn't as easy to say, "well she is really sick, so she really needs this surgery". Not that this isn't true. It just isn't apparent.
I am just saying, in weakness, I think, "does she really have to do this?" "She is doing so well."
I guess though, I understand that she does really need to do this. I just wish there was a way I could communicate it to her.
In one way, I understand that this is just part of her experience. It is not inherently a good or bad thing. But as a parent, I wish I could take on all the suffering for her. As a spiritual practitioner, I really wish I could take on the suffering of all beings. But, this experience, along with much of the current world events, make this aspiration much less abstract than it has been in the past. I suppose this is beneficial, but it is difficult none the less.
Thanks-Michael
I went back to work today. And though I was not thrilled, it was better than agonizing in the surgery waiting room while they cut on Sophia. Sophia's surgery being postponed has me thinking about how mentally prepared I am for it. I think yesterday was a good exercise/dry run for what is inevitable. And though I cannot think of any preparation that I haven't already done. This has left me a little better prepared than I would have been if we were having surgery today.
The hardest part of it, is that Sophia is doing better right now than she ever has. This is great in almost every way that I can think of. But, it prevents me from dealing with the surgery in a way that would be easier. It isn't as easy to say, "well she is really sick, so she really needs this surgery". Not that this isn't true. It just isn't apparent.
I am just saying, in weakness, I think, "does she really have to do this?" "She is doing so well."
I guess though, I understand that she does really need to do this. I just wish there was a way I could communicate it to her.
In one way, I understand that this is just part of her experience. It is not inherently a good or bad thing. But as a parent, I wish I could take on all the suffering for her. As a spiritual practitioner, I really wish I could take on the suffering of all beings. But, this experience, along with much of the current world events, make this aspiration much less abstract than it has been in the past. I suppose this is beneficial, but it is difficult none the less.
Thanks-Michael
Tuesday, September 13, 2005
Surgery is on September 26th.
I just received a call from the CV Surgery nurse. They had just got out of surgery. The surgeon has rescheduled Sophia's surgery for Monday, September 26th.
-Michael
-Michael
Surgery Postponed
Unfortunately the surgery that was supposed to be tomorrow has been postponed. Apparently, a letter regarding pre-op instructions was not sent or lost in the mail. Because of this a medication (aspirin) was not discontinued when it should have been. Because of risk of bleeding, the surgery will be rescheduled later. Possibly early next week.
Thanks for your support-
Michael
Thanks for your support-
Michael
Sunday, September 11, 2005
Surgery Just a Few Days Away
 Hi all.
Hi all.We are just a few days away from surgery and I don't really have any new info to post.
We have spent the last few days letting all the people who Sophia's life has touched visit and spend time with her.
I have spent the whole day, so far, with Sophia cuddling and playing. I just gave her a bath and changed her. I think I am going to spend the evening watching her while my wife cleans the house.
It is funny the different way we deal with stress. I tend to just let everything go to hell, while Patty cleans and orders her environment.
We have pre-op appointments on Tuesday. I will post regarding the details of her surgery after that.
I would like to thank my wife for the incredible job she has done getting and keeping Sophia healthy leading up to this surgery. Sophia has met and exceeded almost every goal we had set leading up to surgery. And this is largely due to Patty's diligence. Sophia is very fortunate to have such a good mom.
Tomorrow is going to be family day. Hopefully, we can get in some real quality time before surgery.
Thanks for comments and support. It means very much to me to receive comments and emails.
And please feel free to ask for elaboration on anything I have posted so far. I try to be comprehensive but it is hard to remember and post all the pertinent details.
Thanks-Michael
Wednesday, September 07, 2005
Impending Surgery
 Hi all.
Hi all.As surgery approaches Patty and I are getting a little more anxious. I think it is perfectly normal, but it is curious nonetheless.
It is hard of course for me to focus all my attention on the matters at home with all the hardship elsewhere. However, being aware that my mind is agitated by my concerns for Sophia, I can see how my feelings in general are magnified regarding other issues in the world.
I think the rational aspects of my thought processes have divorced themselves from the emotional and vice versa. In other words I find myself having emotions run amok without any basis in rational thought and rationality that is cold and nihilistic, desperately needing the warmth of emotion.
I think this is why people turn to spirituality in times like these. When spiritual practice is at its best, it unifies these two seemingly disparate sides of the mind into a balanced whole. In my particular practice it is about the unification of compassion and wisdom. I find it very helpful to use difficult times like these to notice how my mind works with the experience and hopefully find some level of understanding and balance from it.
I know this post is a little bit of a departure from the types of post I have put up thus far. But, I thought it might help me to find that understanding and balance if I posted regarding the issues I wrote about above.
Thanks for your patience-Michael
Sunday, September 04, 2005
Heart Surgery is September 14th

Hi everyone,
I had mentioned in an earlier post, Sophia would be having surgery on September 14th. I will try to take a minute and explain what will happen and why.
So as I have explained Sophia has a CHD called Tetralogy of Fallot with Pulmonary trunk atresia.
I put links (in blue) to diagrams of these conditions in a previous post. Because of the defect to the pulmonary arteries (PAs) she was unable to properly return blood to the lungs to be oxygenated. So in the first surgery, as I explained before, she had a shunt put in that ran from her aorta to the existing PAs. This for the most part stabilized her condition. This is not meant to be a permanent solution by any means and she has done better than expected. The main purpose of this was to allow the combination of time and increased blood flow to result in her PAs growing to a size that would be manageable for a more complete repair. So the idea was to give her as long as the shunt would support her to grow and in turn for the PAs to grow as well.
Sophia sees her cardiologist regularly and he does an echocardiogram to see how her heart is functioning. This is not a high resolution test and I believe takes a great deal of finesse to read accurately. He also measures Sophia's O2 saturation. As we get further away from the first surgery, Sophia's O2 sats begin to decrease. This is expected as the demands of her growing body out grow her shunt. Once this process began her cardiologist performed a heart catheterization to get a more accurate picture of how the vessels around her heart were growing, especially the PAs. At that time the results were shared with the surgeons and it was decided that they had grown enough to operate. But since Sophia was still doing OK, they decided to put the surgery off as long as they could so the PAs might grow even more. Now it is important to note, that the idea was to wait, but to make sure she was not compromised by doing so. In other words, it was important to us and her doctors that the surgery be elective and not emergency.
So on her last cardiologist appointment, Sophia's O2 sats were low enough to indicate we needed to schedule surgery. So we did.
Now here is what is supposed to happen. This is just a general overview. I will provide more detail as I am able.
This will be an open heart surgery. Her first surgery required her chest be cracked open but the heart was not operated on, just the major vessels associated with the heart. This surgery will actually require the heart be operated on.
So as I mentioned in a previous post, Sophia is missing the trunk part of her PAs (if you imagine a "Y", she is missing the vertical part). The trunk is the part that connects to the heart and has a valve in it as well. So the idea is to, take a vessel (probably from a cadaver) and make a conduit from the heart to the PAs as they exist now, replacing the missing trunk.
Sophia also has what is called a "VSD" or ventricular septal defect. This is basically a hole in the wall between her left and right ventricles in the heart. This defect is associated with the tetralogy of fallot. The surgeon believes he can repair this at the same time. This is significant because, it is one less surgery Sophia would require later.
Obviously we are anxious about this impending surgery but if it gets our daughter's heart functioning properly it will be wonderful.
I will post more on this in the days leading up to the surgery. And also try to cover more of the therapies and treatments Sophia has received.
Thanks for reading-Michael
Friday, September 02, 2005
Hurricane Katrina
Hi everyone,
I just wanted to take a moment to ask all the people that may read this blog to do what they can to help support the victims of Hurricane Katrina. I have included a link to the Red Cross donation site below. Give as much as you are able. Even a small amount can make a difference.
-M
Red Cross Hurricane Relief Fund
I just wanted to take a moment to ask all the people that may read this blog to do what they can to help support the victims of Hurricane Katrina. I have included a link to the Red Cross donation site below. Give as much as you are able. Even a small amount can make a difference.
-M
Red Cross Hurricane Relief Fund
First Steps- Ongoing therapy (by Patty)
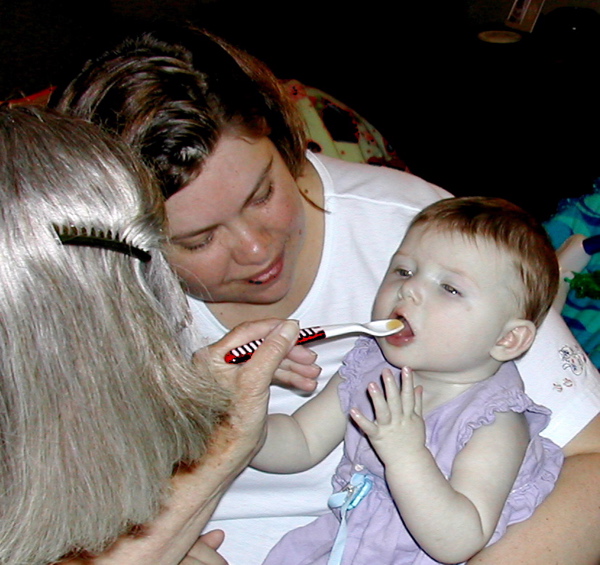 I want to begin this entry by stating that currently Sophia is receiving 4 different types of therapy in regards to physical delays she has due to being hospitalized for so long as an infant and because of her medical condition. Upon discharge, after our daughter had her first heart surgery, the social worker at the children's hospital put us in touch with a state program called First Steps. This is a totally free program that provides various types of therapies to physically and mentally challenged children that are residents of the state of Missouri. Even being a past state employee myself, I had never heard of it prior to this.
I want to begin this entry by stating that currently Sophia is receiving 4 different types of therapy in regards to physical delays she has due to being hospitalized for so long as an infant and because of her medical condition. Upon discharge, after our daughter had her first heart surgery, the social worker at the children's hospital put us in touch with a state program called First Steps. This is a totally free program that provides various types of therapies to physically and mentally challenged children that are residents of the state of Missouri. Even being a past state employee myself, I had never heard of it prior to this.My entire focus of attention since the day we brought Sophia home from the hospital is her full recovery. So naturally Michael and I thought the program would help attain that goal and sounded wonderful (it is).
Soon we met with a representative of the program who did a brief evaluation of Sophia's developmental progress and recommended she see a feeding specialist (because she was not able to swallow) and a physical therapist because she was lagging behind with her motor skills.
So, we began meeting with a feeding specialist who introduced Sophia to various oral stimulation exercises. This lady came to our home weekly for an hour and introduced putting small objects with different textures and tempatures, such as baby toothbrushes and cold baby spoons in Sophia's mouth. This therapist recommended that the hospital conduct a swallow, or "OPM", study to see how her anatomy functions while she swallows. Sophia failed this test miserably. She had had one previous study shortly after surgery while still in the hospital and it went very badly as well. Progress with this therapist was slow, and because of the OPM study she was unwilling to let Sophia have even tiny amounts of food orally. So eventually, we got a new therapist.
This therapist began to slowly introduce baby food in small tastes to our daughter. This was very successful and Sophia now swallows 15 bites of baby food two times a day. I know that this does not sound like much, but we are so proud of her progress.
This new therapist comes twice a week for an hour and works with her speech and language for half of each of her one hour sessions. With this therapy she has learned her first words, mama, lala, nana and yaya. We are working on dada.
One thing to mention before going further is, the great part about all these therapists is they come to your home to do this work and they focus a lot on teaching parents how to continue the therapy in there absence.
Sophia also sees a physical therapist twice a week for 30 minutes. We are so lucky to have such a great PT she bring so much experience with her. This therapist works on skills like sitting up, tummy time, trunk control and muscle tone. Sophia's has made leaps and bounds with her progress in physical therapy. She works really hard for her therapists and enjoys playing with toys on the floor. Recently she has started to sit up independently. This was a huge goal for her.
Our daughter also meets with a occupational therapist. She is also wonderful at her job. She comes for an hour each week. Sophia enjoys this therapy session the most. She works on her fine motor skills. She has improved in the areas of picking up various sized objects with her cute little hands, banging blocks together and using her hands and muscles to help balance herself while sitting.
Lastly, she sees a registered dietitian. Our girl has experienced some major ups and downs with her weight in the last few months. I am happy to say she is doing quite well in this area now. Anyway the dietitian comes every week at the same time and weighs Sophia. This has proven to be quite reassuring to us. Sophia sees so many specialists, doctors and hospital clinics that every time she got weighed at one of these appointments with all these different scales her weight would fluctuate. So it is great to know that her weight is being monitored weekly by the same professional with the same scale to accurately measure her progress.
Sophia has a total of six separate therapy sessions per week. It is a full time job managing the scheduling of the appointments so they coordinate with feedings, baths, doctor appointments and naps. I believe strongly that these amazing therapist have had a tremendous impact on our little girls development. I also feel that after her upcoming heart surgery, she will progress quickly with new found energy. Sophia's therapies are a way of life at our home.
-Patty
Thursday, September 01, 2005
Flickr! Photo Links
I just wanted to point you toward the Flickr! links I have added on the left sidebar.
If you click on any image in the animated one, it will take you to a larger version of that photo.
The other link below the flash one is a direct link to the photo set associated with this blog. I will likely utilize Flickr! for photo posts in the future.
My wife, Patty, is going to write about some of the therapy Sophia receives through an organization called First Steps in tomorrows post.
-M
If you click on any image in the animated one, it will take you to a larger version of that photo.
The other link below the flash one is a direct link to the photo set associated with this blog. I will likely utilize Flickr! for photo posts in the future.
My wife, Patty, is going to write about some of the therapy Sophia receives through an organization called First Steps in tomorrows post.
-M


